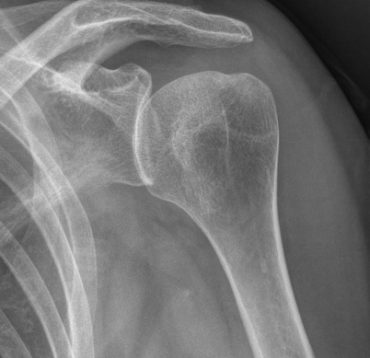
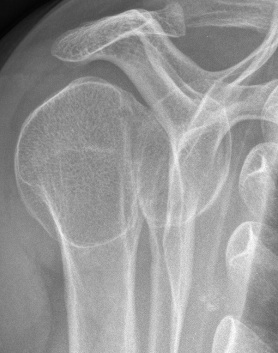
Posterior instability of the shoulder is rare, it represents 10% of the cases of instability in the shoulder (dislocations are mainly anterior).
Anatomically, the humeral head is by nature retroverted, posterior instability does not necessarily require trauma involving a large range of motion (unlike previous dislocations often consecutive to an abduction-external rotation)
Exept trauma, several situations promote posterior instability:
- Epilepsy’s seizures
following a sudden and intense contraction of the muscles with tendency to put the arms in internal rotation, the joint is dislocated towards the back. The associated amnesia of the crisis may mask the notion of trauma. The trauma is so violent that it can also be a dislocation with fracture.
- Anatomical disorders of the bony parts (exageration of the retroversion of the humeral head or of the glenoid).
- Constitutional or pathological joint hyperlaxity (Ehlers Danlos syndrome)