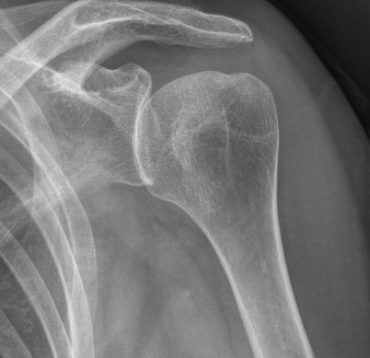
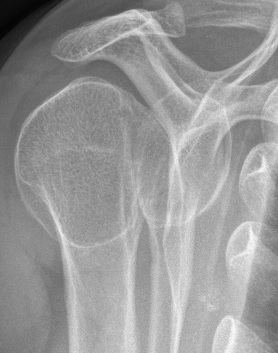
Posterior instability of the shoulder is rare, it represents 10% of the cases of instability in the shoulder (dislocations are mainly anterior).
Anatomically, the humeral head is by nature retroverted, the post instability does not necessarily require trauma involving a large range of motion (unlike previous dislocations often consecutive to a ‘thwarted arm’)