Definition
Osteosynthesis is an intervention aimed at reducing and stabilizing a segment of the skeleton, particularly in the event of a fracture.
Principe
Its principle is to fix the different bone fragments between them and in a good position (the most anatomical possible).
For upper fractures of the humerus it is possible to use pins, screwed plates or screws alone as well as nails (metal rods).
The fractures of the tuberosities can be reinserted in the same way as rotator cuff tendon repairs.
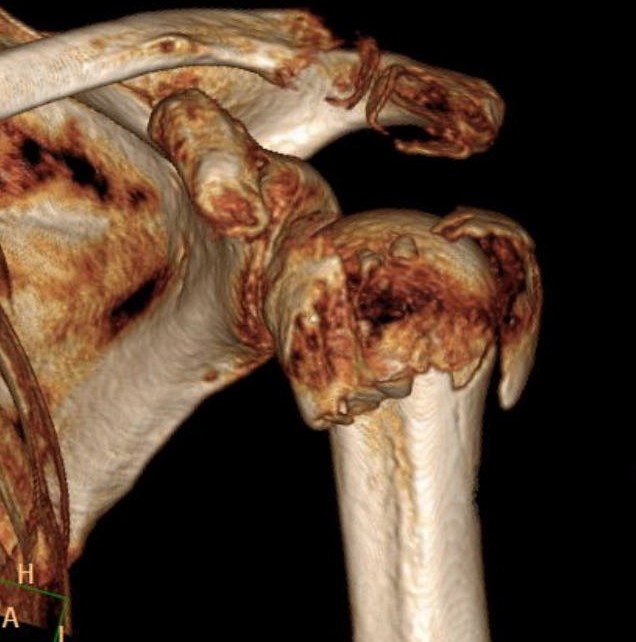
Our technical choice
Each surgeon develops a technique that he then reproduces regularly or will evolve to others if he is not completely satisfied.
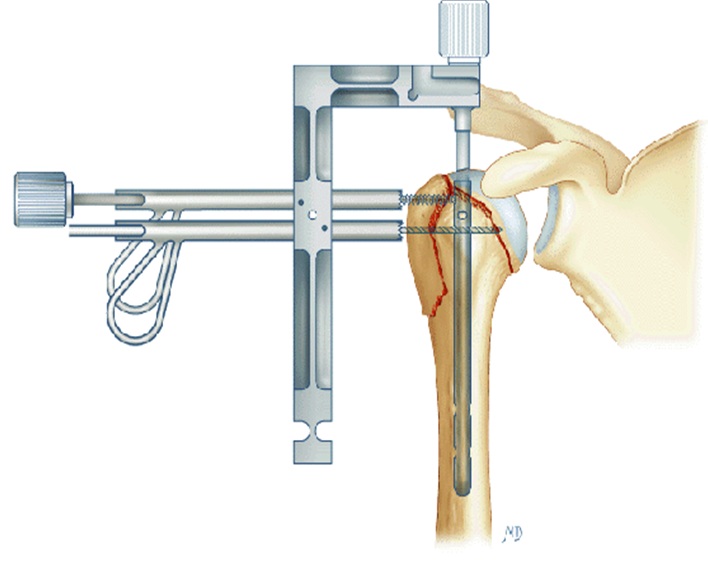
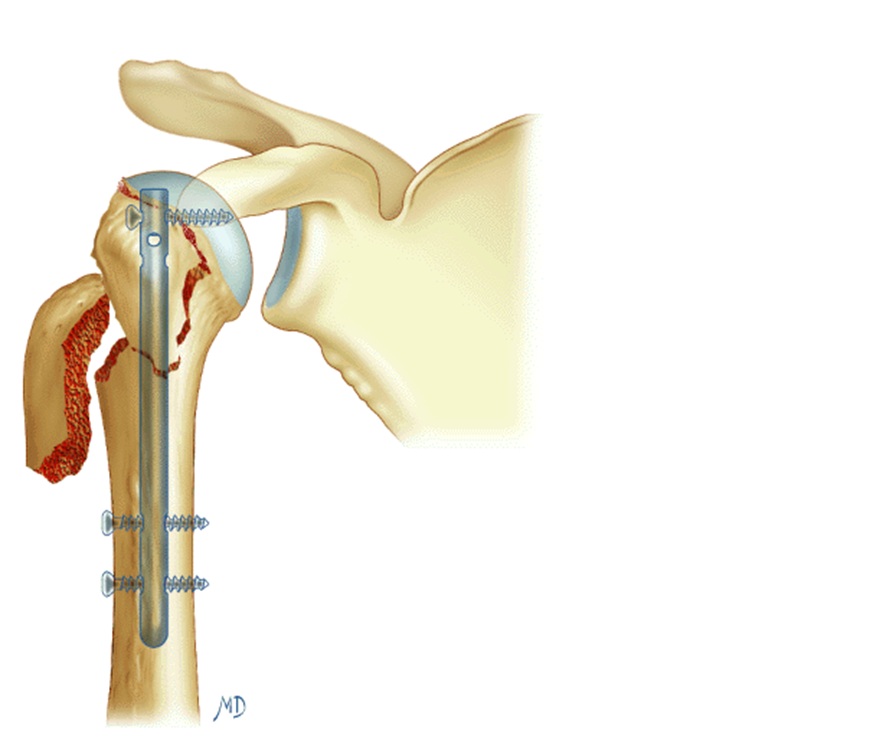
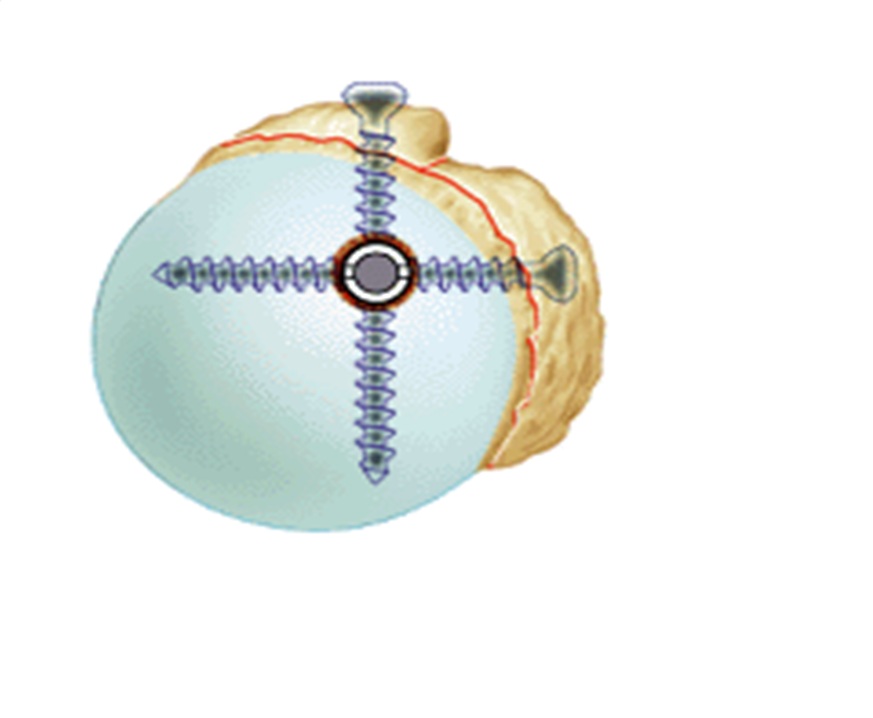
We chose to use the intramedullary nailing, introduced into the head of the humerus and positioned in the hollow of the diaphyseal bone.
It makes it possible to fix the tuberosities with the humeral head and the diaphysis by means of screws and sometimes of bone and tendinous suture threads.
Operative suites
Hospitalization of 48 hours except complications or other associated pathology.
Rest of the arm in a Dujarrier (scarf against scarf) during 4 weeks not strict (according to the opinion of the surgeon)
Immediate physiotherapy usually limited the first month to the pendulum, mobilization of the elbow and lymphatic drainages because of the edema which accumulates around the elbow.
first consultation to 1 month (except J8 fragile assembly) with a radio control, allowing the weaning of immobilization and beginning of the physiotherapist still protected a fortnight.
Consultations 3rd month then 6 months and one year.
Work stopping
manual: between 3 and 6 months (except complication)
sedentary: 6 weeks most often (except complication)
Autonomy
driving car / motorcycle 4 to 6 weeks
dress 2 months, cleaning and carrying loads 3 months
Unsolicited sports: 3 months
(jogging and bike possible before)
Soliciting sports: 6 months
Complications
long and difficult suites:
retractile capsulitis or algodystrophy -> convalescence delay from 12 to 18 months (or more …)
infection on material (re-intervention material ablation, washing and antibiotics)
pseudarthrosis = non-fracture consolidation (re-intervention)
hardware-related gene (re-intervention for ablation)
Convalescence
From 3 to 6 months, the mobility of the shoulder can progress during the year following the intervention.
Thanks to the intervention, we can hope for a better functional result (better mobility) than in the absence of surgery, but sequelae are frequent (limitation of mobility, however, does not interfere with daily life)